A rash on the top of your foot if you have diabetes is a significant concern, often signaling underlying issues related to blood sugar control, circulation, or nerve damage. It’s crucial to identify the specific type of rash, as conditions ranging from fungal infections to diabetic dermopathy require different approaches to prevent complications and promote healing. This guide will help you understand common types, symptoms, and essential care strategies for rashes affecting the diabetic foot.
Understanding Diabetic Foot Rashes

Living with diabetes means paying extra attention to your feet, and for good reason! Your feet are particularly vulnerable to a variety of skin issues, including rashes, that can signal deeper problems related to your condition. Understanding why these rashes occur and how they manifest is the first step toward effective management and prevention.
* Why they occur: High blood sugar can impair immune function, damage nerves, and reduce blood flow, making skin more susceptible to infections and slower to heal.
When your blood glucose levels are consistently high, it creates a cascade of effects throughout your body, directly impacting your skin’s health. Firstly, elevated sugar levels can weaken your immune system, making it harder for your body to fight off common pathogens like bacteria and fungi that might not trouble someone without diabetes. This means a minor cut or irritation can quickly escalate into a full-blown infection. Secondly, sustained high blood sugar can damage nerves (neuropathy), particularly in your feet. This damage can lead to a loss of sensation, meaning you might not feel a developing rash, blister, or cut until it’s quite advanced. Lastly, diabetes can restrict blood flow to your extremities (peripheral artery disease), reducing the supply of oxygen and nutrients essential for healthy skin and wound healing. When blood flow is compromised, even a small rash struggles to heal, increasing the risk of infection and serious complications.
* Common areas affected: While various parts of the body can develop diabetic skin conditions, the feet are particularly vulnerable due to pressure, moisture, and potential nerve damage.
While diabetes can affect skin all over your body, your feet are truly on the front lines when it comes to skin problems. They endure constant pressure from walking and standing, are often enclosed in shoes creating warm, moist environments perfect for fungal growth, and are frequently areas where nerve damage first manifests. This combination makes the top of your foot, between your toes, and your soles prime locations for developing rashes and other skin issues. You might not feel the subtle rub of a shoe, the dampness from sweat, or the start of a small cut, allowing problems to progress unnoticed until they become more severe.
* Variety of presentations: Rashes can manifest as dry patches, blisters, red spots, discolored areas, or open sores.
Diabetic foot rashes aren’t a one-size-fits-all problem; they come in many different forms. You might notice areas of unusually dry, flaky skin that could be a sign of poor circulation or early neuropathy. Blisters, which can be small and irritating or surprisingly large and painless, are another common presentation. Red spots, either isolated or clustered, might indicate inflammation or the start of an infection. Sometimes, you’ll see areas of discolored skin, such as light brown, reddish, or even purplish patches, which can signify different underlying conditions. In more advanced or neglected cases, rashes can progress to open sores or ulcers, which are particularly concerning and require immediate medical attention due to the high risk of infection. Each presentation offers clues about the potential cause, underscoring the importance of careful observation.
Identifying Common Types of Rashes on the Diabetic Foot
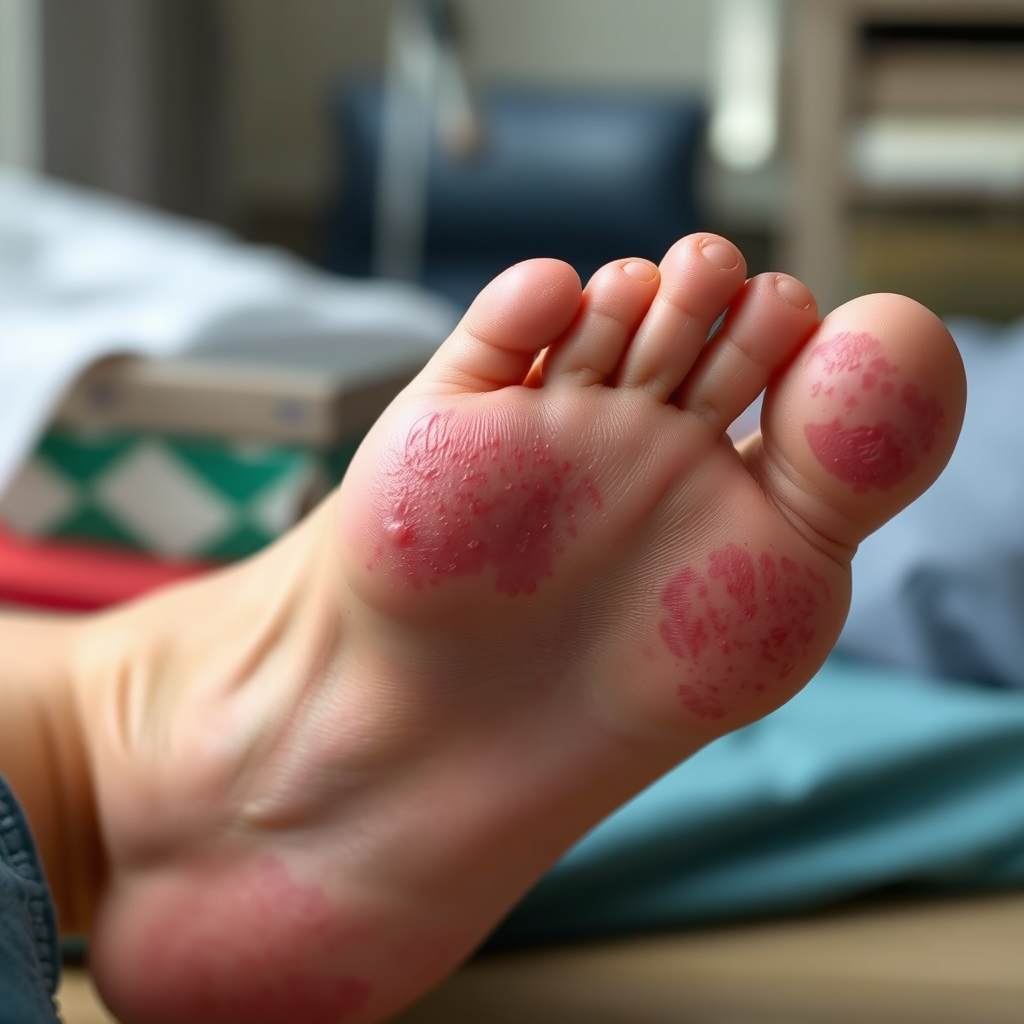
Pinpointing the exact type of rash you’re dealing with is vital because different conditions require different care approaches. While your doctor will provide a definitive diagnosis, knowing what to look for can help you communicate your symptoms effectively and understand the potential causes.
* Diabetic Dermopathy (Shin Spots): Small, round, light brown or reddish patches, often appearing on the shins but can occur on the feet. They are harmless but indicate microvascular changes.
Often affectionately called “shin spots” because of their common location, diabetic dermopathy can also make an appearance on the tops of your feet. These spots are typically small, round or oval, and start off reddish before fading to a light brown, almost like age spots. They aren’t itchy, painful, or open sores, but rather a benign skin condition resulting from changes in the small blood vessels (microvasculature) that supply the skin. While they don’t usually require treatment themselves, their presence is a strong indicator that you’ve been living with diabetes for some time and might have some microvascular changes occurring elsewhere in your body. It’s a gentle reminder to recommit to excellent blood sugar control!
* Fungal Infections (Athlete’s Foot): Caused by fungi thriving in warm, moist environments, presenting as itching, redness, scaling, or blistering, often between toes but can spread to the top of the foot.
Athlete’s foot, or tinea pedis, is a common fungal infection that can be particularly problematic for individuals with diabetes. These fungi adore warm, dark, and moist environments – precisely what your feet encounter inside shoes. While it often starts with itching, redness, and scaling between the toes, it can easily spread to the top of your foot, causing generalized redness, dry flakes, or even small, fluid-filled blisters. The skin might look macerated (whitish and soggy) in moist areas. Due to impaired immune function and poor circulation, diabetic feet are more susceptible to these infections, and they can be harder to clear up, increasing the risk of secondary bacterial infections if the skin barrier is compromised by scratching or cracking.
* Bacterial Infections (Cellulitis, Erysipelas): Red, swollen, warm, and painful areas, potentially with pus or fever, requiring urgent medical attention.
Bacterial infections of the skin, such as cellulitis or erysipelas, are serious concerns, especially for someone with diabetes. These infections can develop rapidly and spread quickly. You’ll typically notice a localized area of skin that becomes intensely red, swollen, warm to the touch, and often very painful. Unlike fungal infections that might cause scaling, bacterial infections usually present with a smooth, shiny, and stretched appearance of the skin. Pus might be present, and you could experience systemic symptoms like fever, chills, and general malaise. Even a tiny break in the skin, like a small cut, blister, or even severe dryness, can provide an entry point for bacteria. Given the potential for rapid progression and serious complications like foot ulcers or bloodstream infections, any suspected bacterial infection requires urgent medical attention.
* Diabetic Blisters (Bullosis Diabeticorum): Large, painless blisters that resemble burn blisters, typically resolving on their own but prone to infection if broken.
Bullosis diabeticorum, or diabetic blisters, are a less common but distinctive type of skin condition. These aren’t your typical small friction blisters; they can be quite large, sometimes several inches in diameter, and often appear suddenly on the top of the foot, toes, or lower legs. What’s often surprising is that they are usually painless and appear without any obvious injury or trauma. They look like severe burn blisters, filled with clear fluid, but the surrounding skin is typically normal. While these blisters often heal on their own within a few weeks without scarring, they pose a significant risk if they break open. An open blister creates an entry point for bacteria, potentially leading to a serious infection in a diabetic foot that is already vulnerable. It’s crucial not to pop them yourself and to seek medical advice for proper care.
Recognizing Symptoms and Warning Signs
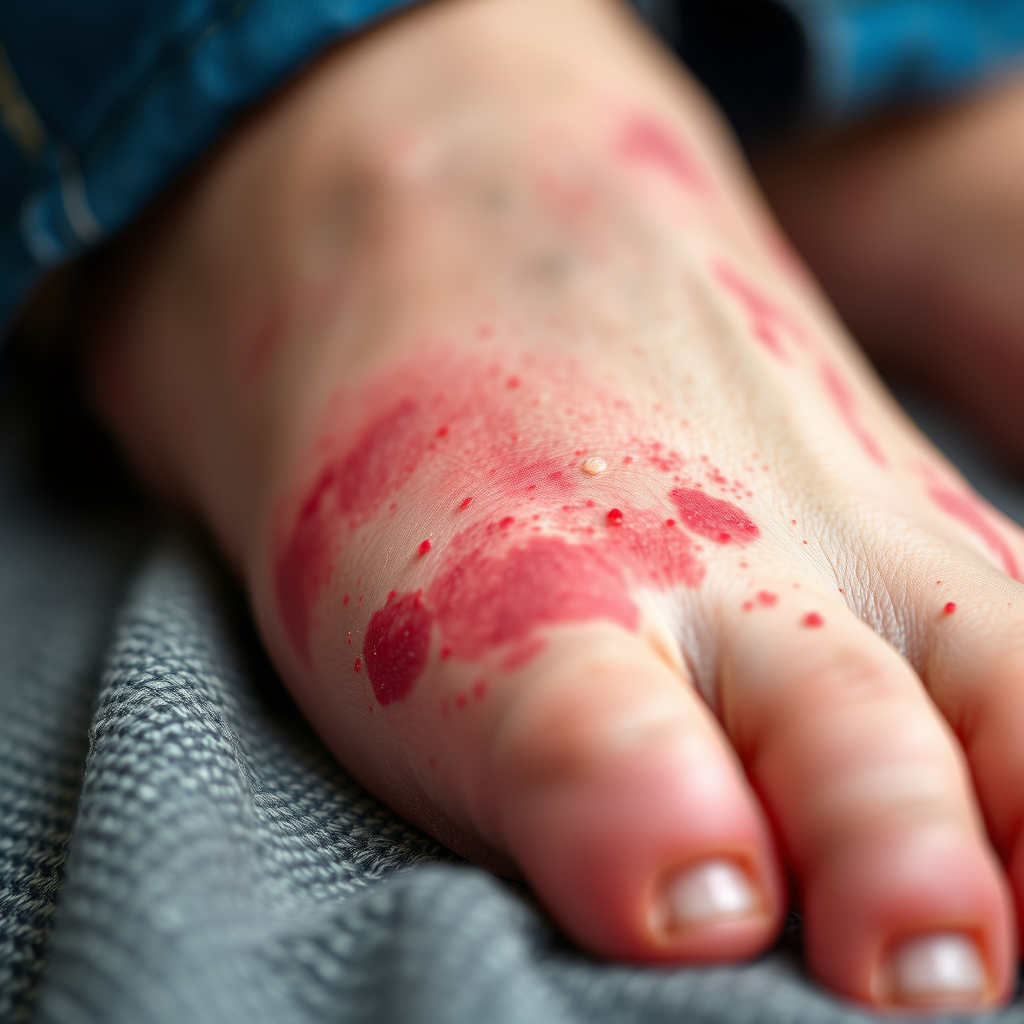
Early detection is your best defense against complications when it comes to diabetic foot rashes. Being proactive about observing your feet and understanding what to look for can make a world of difference in managing your health.
* Visual cues: Look for unusual redness, discoloration (brown, purple), scaling, cracking, or blistering on the top of your foot.
Your eyes are your primary tool for daily foot inspection. Make it a routine to visually examine the top of your feet, between your toes, and your soles. Pay close attention to any areas of unusual redness that wasn’t there before – it could indicate inflammation or the start of an infection. Be aware of any discoloration; light brown patches might suggest dermopathy, while purplish or bluish hues could signal poor circulation. Scaling, flakiness, or peeling skin often points to dryness or a fungal infection, while cracking skin creates openings for bacteria. And, of course, any new blisters, whether small and irritating or large and painless, should always be noted. Remember, even subtle changes can be significant.
* Sensory changes: Pay attention to itching, burning, pain, warmth, or a new loss of sensation in the affected area.
While visual cues are important, sensory changes provide another layer of information. Itching is a classic sign of fungal infections or dry skin, while a burning sensation might accompany nerve irritation or inflammation. Pain, especially if it’s localized, intense, or throbbing, is a clear warning sign of a potential infection or injury. New warmth in a specific area, compared to the rest of your foot, also strongly suggests inflammation or infection. Conversely, a new or worsening loss of sensation (numbness) in the area of a rash is very concerning, as it means you might not feel pain or discomfort, allowing a problem to become severe before you’re even aware of it. This highlights the importance of combining visual checks with a general awareness of how your feet feel.
* Progressive symptoms: Any rash that grows, doesn’t heal, or is accompanied by fever, pus, or severe pain needs immediate evaluation.
Some rashes might start small and seem benign, but it’s their progression that truly flags them as dangerous. If you notice a rash that is steadily growing in size, spreading to other areas, or simply not improving after a few days of careful home care, it’s time to see a doctor. Even more critically, if a rash is accompanied by systemic symptoms like a fever, chills, or a general feeling of being unwell, it could indicate a spreading infection that requires immediate medical intervention. The presence of pus, foul odor, or increasingly severe pain around the rash also signals a serious problem that cannot wait. Trust your instincts; if something feels wrong or is getting worse, seek professional help without delay.
Effective Care and Treatment Approaches
Taking care of a diabetes-related foot rash involves a multi-pronged approach, integrating careful self-management with targeted medical treatments. The cornerstone of all care, however, always begins with your overall diabetes management.
* Blood sugar management: Maintaining optimal blood glucose levels is fundamental to preventing and healing diabetic skin conditions.
This cannot be stressed enough: achieving and maintaining excellent blood sugar control is the single most impactful thing you can do for your skin health, especially concerning rashes and wound healing. High blood glucose fuels inflammation, impairs immune function, and slows down your body’s natural healing processes. By keeping your A1c in your target range and regularly monitoring your daily blood sugars, you create a healthier internal environment. This not only makes you less susceptible to infections and skin conditions in the first place but also significantly improves your body’s ability to heal any rashes or sores that do develop. Think of stable blood sugar as the foundation upon which all other foot care efforts are built.
* Topical medications: Antifungal creams for fungal infections, corticosteroid creams for inflammatory rashes, or prescribed antibiotics for bacterial infections.
Depending on the type of rash, your doctor might prescribe various topical medications. For fungal infections like athlete’s foot, over-the-counter or prescription antifungal creams, sprays, or powders are often effective. It’s important to use them consistently as directed, usually for a period even after symptoms disappear, to ensure the infection is fully eradicated. For inflammatory rashes that aren’t infected, such as certain types of dermatitis, a mild corticosteroid cream might be prescribed to reduce redness and itching. For bacterial infections, topical antibiotic creams might be used for minor issues, but often oral antibiotics are necessary to tackle deeper infections. Never self-prescribe strong medications; always consult your healthcare provider to ensure you’re using the correct product for your specific condition.
* Wound care: Keep the rash clean and covered if open, using appropriate dressings as advised by a healthcare professional to prevent secondary infections.
If your rash has progressed to an open sore, blister, or broken skin, diligent wound care is paramount. The primary goals are to keep the area clean, protect it from further injury, and prevent infection. This usually involves gently cleaning the wound with mild soap and water or a saline solution, then applying a sterile, non-stick dressing. The type of dressing can vary widely depending on the wound’s depth, exudate, and location, ranging from simple gauze to advanced moisture-retaining dressings. It’s crucial to follow your healthcare professional’s specific instructions for dressing changes and wound management. Attempting to manage complex or deep wounds yourself can lead to serious complications. Always seek professional guidance for open wounds on a diabetic foot.
Preventing Foot Rashes and Promoting Foot Health
Prevention is truly the best medicine when it comes to diabetic foot health. Establishing a routine of proactive care can significantly reduce your risk of developing rashes and other complications, keeping your feet happy and healthy.
* Daily foot inspections: Regularly check your feet (or have a loved one help) for any cuts, blisters, redness, swelling, or changes in skin integrity.
Make daily foot checks a non-negotiable part of your routine. This means taking a few minutes each day to thoroughly examine every part of your feet – the tops, bottoms, sides, and especially between your toes. Use a mirror if needed, or ask a trusted family member to help if reaching or seeing your feet is difficult. You’re looking for anything out of the ordinary: any new cuts, scrapes, blisters, calluses, redness, swelling, changes in skin color, warmth, or even ingrown toenails. Early detection allows you to address minor issues before they escalate into serious problems. This vigilance is your first line of defense!
* Proper foot hygiene: Wash feet daily with mild soap and warm water, dry thoroughly (especially between toes), and apply moisturizer to prevent dry skin (avoiding between toes).
Good foot hygiene is foundational to preventing rashes. Wash your feet daily with a mild soap and lukewarm water – never hot, as neuropathy can make it hard to gauge temperature. After washing, it’s absolutely critical to dry your feet thoroughly, paying special attention to the areas between your toes. Leaving moisture there creates a perfect breeding ground for fungal infections. Once dry, apply a good quality moisturizer to the tops and soles of your feet to prevent dry, cracked skin, which can lead to openings for infection. However, avoid applying moisturizer between your toes, for the same reason you want to dry that area meticulously.
* Appropriate footwear: Wear well-fitting, comfortable shoes and seamless socks to prevent friction and pressure points, changing socks if they become damp.
What you put on your feet matters immensely. Invest in well-fitting, comfortable shoes that provide good support and have ample room in the toe box. Avoid shoes that are too tight, rub, or pinch, as these can cause blisters, calluses, and pressure sores that can easily become infected. Look for shoes made of breathable materials. Equally important are your socks: choose soft, seamless socks made from moisture-wicking materials like cotton blends or specialized diabetic socks. Seamless designs prevent irritation, and moisture-wicking fabrics help keep your feet dry. Always change your socks immediately if they become damp from sweat or other moisture to maintain a dry, healthy environment for your feet.
When to Seek Professional Medical Care
While self-care and prevention are powerful tools, knowing when to call in the experts is crucial for avoiding serious complications associated with diabetic foot rashes. Never hesitate to seek professional advice if you have concerns.
* Persistent or worsening rash: If a rash doesn’t improve with home care within a few days, or if it spreads or becomes more painful.
You might try some basic home care for a minor rash, like keeping it clean and dry, or using an over-the-counter cream for suspected dryness. However, if you don’t see any improvement within a few days, or if the rash starts to spread, gets larger, becomes more intensely red, or increases in pain, it’s a clear sign to contact your doctor. These are indicators that the problem might be more serious than initially thought, or that your home treatment isn’t sufficient. Delaying professional evaluation can lead to the rash becoming more severe and potentially harder to treat.
* Signs of infection: Redness, swelling, warmth, pus, fever, or chills accompanying the rash warrant immediate medical attention.
This is a critical point: any sign of infection accompanying a rash on your diabetic foot requires immediate medical attention. Look out for increasing redness that spreads beyond the rash itself, new or worsening swelling, an area that feels unusually warm to the touch, or the presence of pus or a foul odor. Systemic symptoms like a fever (even a low-grade one) or chills are also strong indicators of a spreading infection that could be serious. Do not wait for your next routine appointment; contact your doctor, a podiatrist, or seek urgent care immediately. These symptoms can signal a rapidly progressing infection that, if left untreated, can lead to severe complications.
* New or unusual symptoms: Any new rash, blister, or skin change on your feet should be discussed with your doctor or a podiatrist.
Given the unique vulnerabilities of diabetic feet, it’s always best to err on the side of caution. If you notice any new rash, blister, unusual spot, or change in the skin on your feet that you haven’t seen before, or that concerns you in any way, don’t try to self-diagnose or wait to see if it goes away. A quick call or visit to your doctor or a podiatrist (a foot care specialist) can provide peace of mind and ensure prompt diagnosis and treatment if needed. They are experts in identifying the specific type of rash and guiding you on the best course of action to protect your foot health.
Managing a diabetes rash on the top of your foot requires diligent self-care and prompt medical attention. By staying informed about the symptoms, understanding potential causes, and adhering to a comprehensive foot care routine, you can significantly reduce your risk of complications. Always consult your healthcare provider at the first sign of a persistent or worsening rash to ensure proper diagnosis and treatment. Your feet work hard for you every day; let’s give them the care they deserve!
Frequently Asked Questions
What does a diabetes rash on top of the foot look like?
A diabetes rash on the top of the foot can manifest in various ways, often appearing as dry, scaly patches, red or discolored areas, or small, itchy bumps. Common conditions include diabetic dermopathy (brownish, coin-shaped lesions), eruptive xanthomatosis (firm, yellow, pea-sized bumps with red halos), or fungal infections like athlete’s foot which can cause scaling and redness. It’s crucial to observe if the skin is breaking down, blistering, or showing signs of infection.
Why do people with diabetes get rashes on their feet?
People with diabetes are more prone to developing rashes on their feet due to several factors, including poor circulation and nerve damage (neuropathy) which impair skin healing and sensation. High blood sugar levels weaken the immune system, making individuals more susceptible to bacterial and fungal infections, which often present as rashes. Additionally, dry skin, a common diabetic complication, can lead to cracks and openings that allow pathogens to enter, contributing to foot rash development.
How can I treat a diabetic rash on my foot?
Treating a diabetic rash on your foot typically involves addressing the underlying cause and maintaining meticulous foot care. For fungal infections, antifungal creams or oral medications prescribed by a doctor are essential, while bacterial rashes may require antibiotics. It is vital to keep the affected area clean and dry, apply any prescribed topical treatments, and ensure blood sugar levels are well-controlled to support healing and prevent recurrence of the diabetes rash.
When should I see a doctor for a rash on my foot if I have diabetes?
You should promptly see a doctor for any rash on your foot if you have diabetes, especially if it doesn’t improve with basic care, spreads, becomes painful, blisters, or shows signs of infection like redness, swelling, warmth, or pus. Given the risks of complications such as ulcers and infections in diabetic patients, early diagnosis and treatment of a foot rash are crucial to prevent more serious health issues and ensure proper healing.
What’s the best way to prevent diabetic foot rashes?
The best way to prevent diabetic foot rashes involves meticulous daily foot care and excellent blood sugar management. Regularly inspect your feet for any changes, wash them daily with mild soap and warm water, and dry thoroughly between toes. Wear well-fitting, breathable shoes and moisture-wicking socks, and moisturize dry skin, avoiding between the toes, to keep the skin barrier healthy and reduce susceptibility to infections and irritation that can lead to a diabetes rash.
References
- https://www.aad.org/public/diseases/a-z/diabetes-skin-problems
- https://my.clevelandclinic.org/health/articles/10978-diabetic-skin-conditions
- Vitamin B-12 injections for weight loss: Do they work? – Mayo Clinic
- Diabetes & Foot Problems – NIDDK
- https://medlineplus.gov/diabeticfoot.html
- Diabetic dermopathy
- Diabetic foot
- https://diabetes.org/health-wellness/diabetes-skin-care
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8331566/